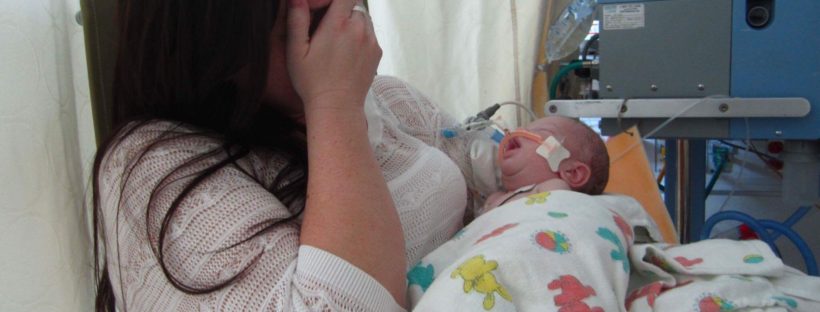
by Kimberly Cartwright
My story is unremarkable but important to tell, because we are often led to believe that it should be remarkably rare.
In 2013 I had my first child, a son. I researched and knew I wanted to breastfeed him, as breast milk is the recommended food for babies. There are so many benefits to baby and mother if you nurse, so of course I wanted to try it out. I have to admit that was a big push to learn all about it and make it work; and we did make breastfeeding work for fourteen months. Then in 2016 I had my second and third children, my twin daughters. I knew I wanted to breastfeed again. The cost benefit for me personally was huge, especially for two babies. But nursing two babies at once–that’s a lot! There are a lot of reasons breastfeeding doesn’t work, and you double those when there are two babies. I was determined to do my best though.
My girls were born at 36 and a half weeks. Early by the forty week schedule, but basically on time for twins. (Full term for twins is considered 37 weeks.) They were right on target for identicals. I was worried they wouldn’t be able to latch or just wouldn’t nurse well. Imagine my relief when shortly after both girls were born, they both latched right on and were nursing away. They knew what to do and we didn’t have any problems. The only issue was with their blood sugar. They were still a bit early and of course small. As per the protocol of the hospital I was at, the girls had to have their blood sugar checked with every feed. They did pretty well, but their numbers weren’t as high as the doctors and nurses would have liked. The nurses offered me a simple solution–after I nursed we were to give the girls supplemental formula. It can take a few days for a mother’s milk to come in. Yes, my girls were getting colostrum, but we were concerned that I wasn’t able to provide enough in terms of volume for two babies. For the two days we were in the hospital we offered enough formula after each nursing session to keep their blood sugar levels normal and safe. Once we got the girls home my milk came in. Fast forward thirteen months later and we are still nursing. Continue reading