My son will be three months old tomorrow, and I’m reflecting on our nursing journey with gratitude. I had infertility and recurrent pregnancy loss before having him, and (after two rounds of IVF and six embryo transfers), he was born at 35 weeks. So we had a lot working against us for successful breastfeeding, but I wanted to try breastfeeding, and I was ready to advocate for myself and the baby if needed in the hospital since I knew I had significant risk factors for delayed onset of milk.
The first day he latched on right away but was so vigorous that he completely tore up my nipples. I was bruised and blistered and bleeding. The lactation consultant and nurses in the hospital were amazing and reaffirmed my desire to breastfeed but encouraged me to feel good about supplemental formula feeding for a few days until my milk came in. They were cognizant of my very sore nipples, limited our nursing time, and helped me get a better latch—and we did—and it improved even more with a corrected latch for each feeding. They gave me so much confidence by keeping my baby fed (he was only 35 weeks) while managing my nipple pain and appropriate stimulation for milk production. The pediatrician referred me to an ENT for a suspected tongue tie, though it turns out his tongue was fine.

They gave me so much confidence by keeping my baby fed (he was only 35 weeks) while managing my nipple pain and appropriate stimulation for milk production.
The lactation consultant and one angel nurse who was also a lactation consultant gave me individualized attention and support. I know now how lucky I was to have such nonjudgmental health care professionals who never shamed me or made me feel guilty for having difficulty early on and for using supplemental formula.
Even the World Health Organization concludes the addition of artificial milk supplementationprobably makes little or no difference to breastfeeding at discharge compared to those who were not supplemented.
The question is how did the very low quality of evidence turn into moderate-quality evidence for exclusive breastfeeding, particularly when the evidence showed improvement of breastfeeding rates in supplemented breastfed newborns?
If we had never fed formula the first few days, we never would have been successful with breastfeeding because I would have stopped from the pain, and my baby would not have been safely fed while waiting for my milk to come in. It’s so wonderful that professionals are interested in safe breastfeeding instead of pressuring every mother to exclusively breastfeed, despite the pressure to meet hospital exclusive breastfeeding rates at discharge.
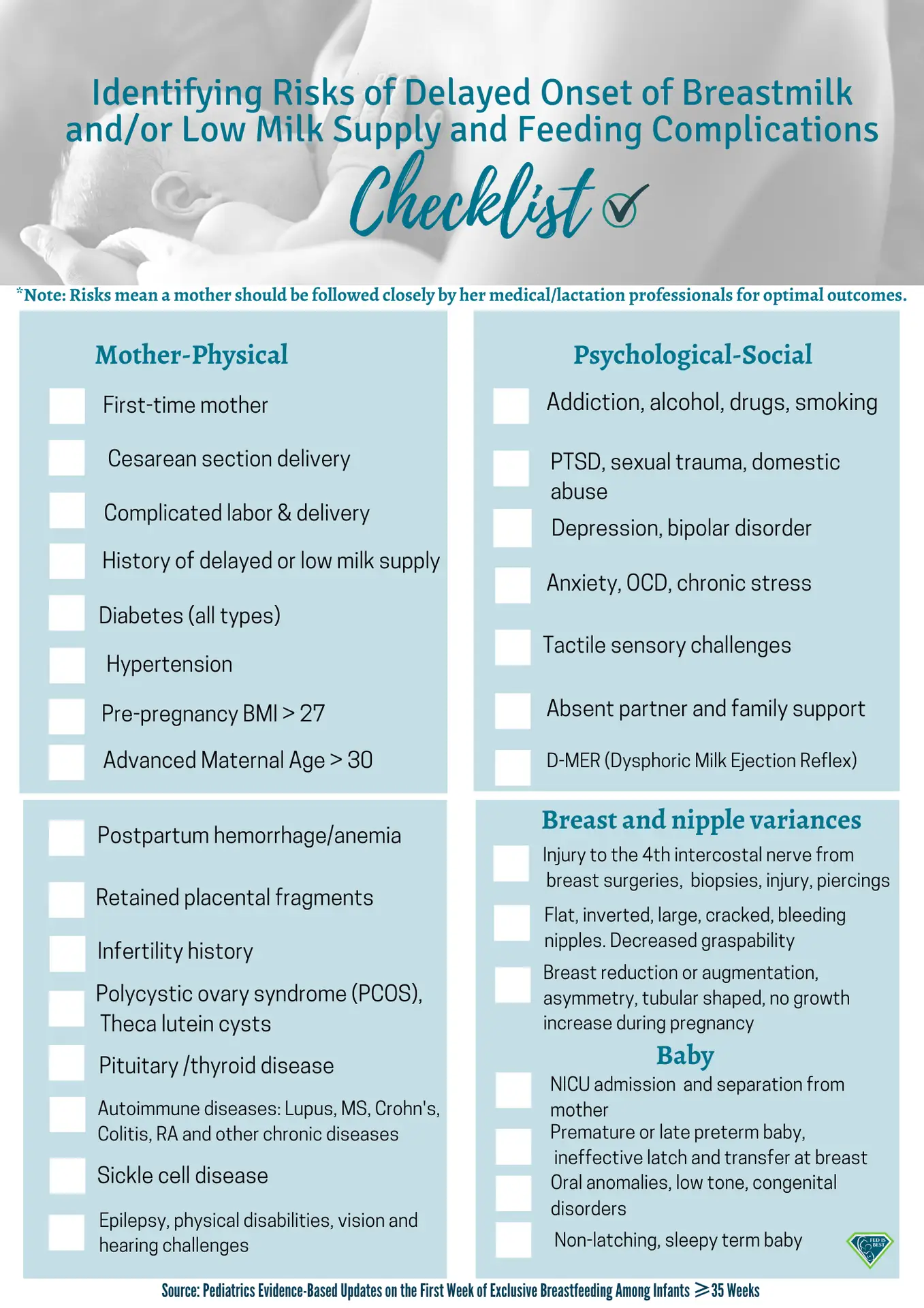
I want to thank the Fed Is Best Foundation’s support group for cultivating a wonderfully supportive space for parents to feel confident about however they end up feeding their babies. That’s where I was initially informed about how to breastfeed my baby safely. I followed their breastfeeding plan, and the first step was to identify my potential risk factors for delayed onset or low milk supply and how to navigate those first five days before I had enough milk to feed my baby fully. We have exclusively breastfed from when my milk came in, and I have a 200 oz freezer stash to help support us in continuing when I return to work in three months. Fed is Best’s educational resources gave me the confidence I needed as a new mother, and I am very thankful.

-Evalyn Patterson
Click here for our free feeding plan.
Click here to join our Fed Is Best Support Group
Additional resources:
How To Prepare For Supplementing When Breastfeeding Your Baby In The Hospital
Feed Your Baby—When Supplementing Saves Breastfeeding and Lives
I Didn’t Make Enough Milk Like So Many Other Moms: Supplementing Saved My Breastfeeding and My Son
Our Close Call with Our Baby’s Life While Exclusively Breastfeeding Haunts Us
If I Had Given Him Just One Bottle, He Would Still Be Alive.
NICU Nurse Discloses Newborn Admission Rates From Breastfeeding Complications in BFHI Unit
We believe all babies deserve to be protected from hunger and thirst every single day of their life and we believe that education on Safe Infant Feeding should be free. If you would like to make a donation to support the Fed is Best Foundation’s mission to teach every parent Safe Infant Feeding, please consider making a one-time or recurring donation to our organization. We do not accept donations from breast- or formula-feeding companies and 100% of your donations go toward these operational costs. All the work of the Foundation is achieved via the pro bono and volunteer work of its supporters.
Please help our advocacy and consider donating. Every penny counts!
Click here to Donate to Fed Is Best Foundation

