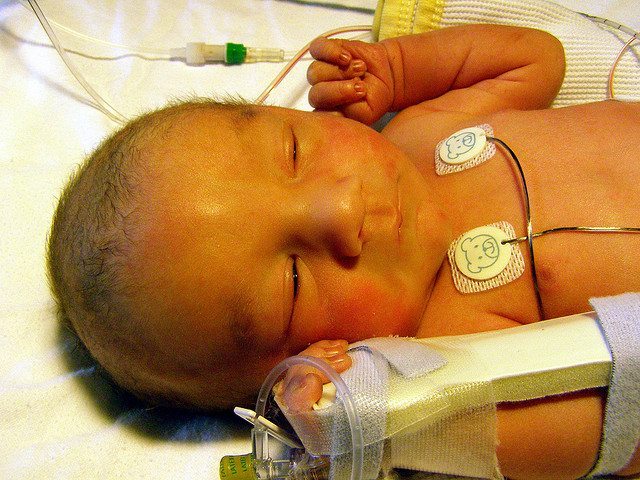
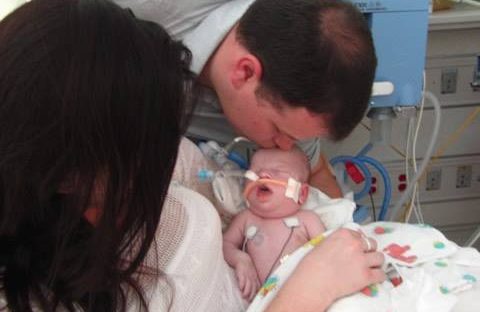
A key recommendation of the 1989 World Health Organization Ten Steps to Successful Breastfeeding which guides the Baby-Friendly Hospital Initiative (BFHI) is: “give infants no food or drink other than breast-milk, unless medically indicated.” This has led to serious complications from accidental starvation of babies, including dehydration, hyperbilirubinemia (jaundice) and hypoglycemia (low blood sugar) — known causes of infant brain injury and permanent disability. Last week, the WHO issued draft revised breastfeeding guidelines, failing to revise this recommendation. These guidelines define the standard of care for breastfeeding management in all healthcare facilities worldwide. Nearly 500 U.S. hospitals and birthing centers and thousands more worldwide that meet the criteria of the BFHI are certified as Baby-Friendly, adhering to the application of the WHO’s Ten Steps.
On Sept. 22, 2017, senior members of the Fed is Best Foundation, and guests including a neonatologist from a leading U.S. tertiary care hospital and a pediatric endocrinologist, Dr. Paul Thornton, M.D, from Cook Children’s Hospital Fort Worth, lead author of the Pediatric Endocrine Society’s newborn hypoglycemia guidelines, met via teleconference with top officials of the WHO Breastfeeding Program: Dr. Laurence Grummer-Strawn, Ph.D., Dr. Nigel Rollins, M.D. and Dr. Wilson Were, M.D. to express their concerns about the complications arising from the BFHI Ten Steps and to ask what, if any, monitoring, research, or public outreach the WHO has planned regarding the risks of accidental starvation of exclusively breastfed newborns. The Foundation members who attended were 1) Christie del Castillo-Hegyi, MD, Co-Founder, 2) Jody Segrave-Daly, RN, IBCLC, Co-Founder, 3) Julie Tibbets, JD, Partner at Alston & Bird, LLP, Pro-Bono Attorney for the Foundation, 4) Brian Symon, MD, Senior Advisor, and 5) Hillary Kuzdeba, MPH, former quality improvement program coordinator at a children’s hospital, managing infant feeding projects and Senior Advisor.
Emails confirming meeting between the WHO and the Fed is Best Foundation available here.
Continue reading →