The first weeks of our baby’s life are hazy, but I remember Meredith’s gasps of pain when she tried to nurse. I remember that the baby kept coming off the breast and crying and we had to get her back on. It was a constant struggle of trying to get the baby latched, having to break her latch because of the pain, then her falling asleep, unlatching, then waking up and crying. It was a seemingly endless cycle.
When we brought the baby home from the hospital, she was crying and we couldn’t get her to stop. I realized she was hungry and I gave her a bottle of formula. She drank down four ounces, stopped crying, and went to sleep. I felt relieved because I was able to make my baby happy and comfortable. I told Meredith that the baby drank 4 ounces of formula and she said that was impossible, because an infant’s stomach can only hold 5 ml, according to the nurse who taught our breastfeeding class. We both now know that is untrue.
The next day, we went to the lactation consultant at the hospital. She told us to supplement with formula, but to give no more than 5 ml at once with a syringe—no bottles. She said the baby’s stomach could only hold 5 ml (our baby was 4 days old) and we should feed her with a syringe to avoid nipple confusion. The baby sucked those 5 ml down so quickly, it was ridiculous. I knew that she needed more than 5 ml, but I didn’t feel qualified to disagree with the lactation consultant. Because she worked at the hospital, I assumed she was giving evidence-based advice. So we fed the baby 5 ml at a time with a syringe. When one syringe-full was insufficient to sate the baby, I often fed her multiple syringes at a time, even though I felt like it was wrong to do so.
The lactation consultant also suggested that Meredith start pumping, so I bought a pump. The lactation consultant really didn’t give any instructions for pumping other than to do it, so when Meredith wasn’t breastfeeding, she was pumping but she hated it.
A couple of days later, Meredith’s milk still had not “come in,” and she was still in agonizing pain every time she nursed. So we went back to the lactation consultant. She recommended a supplemental nursing system (SNS), which is a bag of formula with a tube that attaches to the mother’s nipple. The baby stimulates the nipple while getting formula from the tube. We bought the SNS also rented a hospital pump, which the lactation consultant said would work better than the one I bought. She told my wife to take fenugreek, an herb which supposedly increases milk supply. I went out and got the fenugreek capsules. All they did was make my wife smell like weird maple syrup. We later learned that large amounts of fenugreek can interfere with medication used for hypothyroid (which my wife has), thus lowering a woman’s supply.
We dutifully used the SNS to feed our baby. My job was to tape the tube to my wife’s nipple, which was much more difficult than it sounds, because I had to get it taped at just the right place, while formula was dripping out and my wife and baby were crying.
You then must manage to get the tube and the nipple into the baby’s mouth when she latches. It was like trying to shove a string into the baby’s mouth at just the right moment. From start to finish, it took us an hour to feed the baby using the SNS. Then we slept for an hour and had to wake up and do it all over again. When Meredith was too exhausted to get up, I fed the baby by taping the SNS tube to my finger. We were all frustrated, tired, miserable, and exhausted.
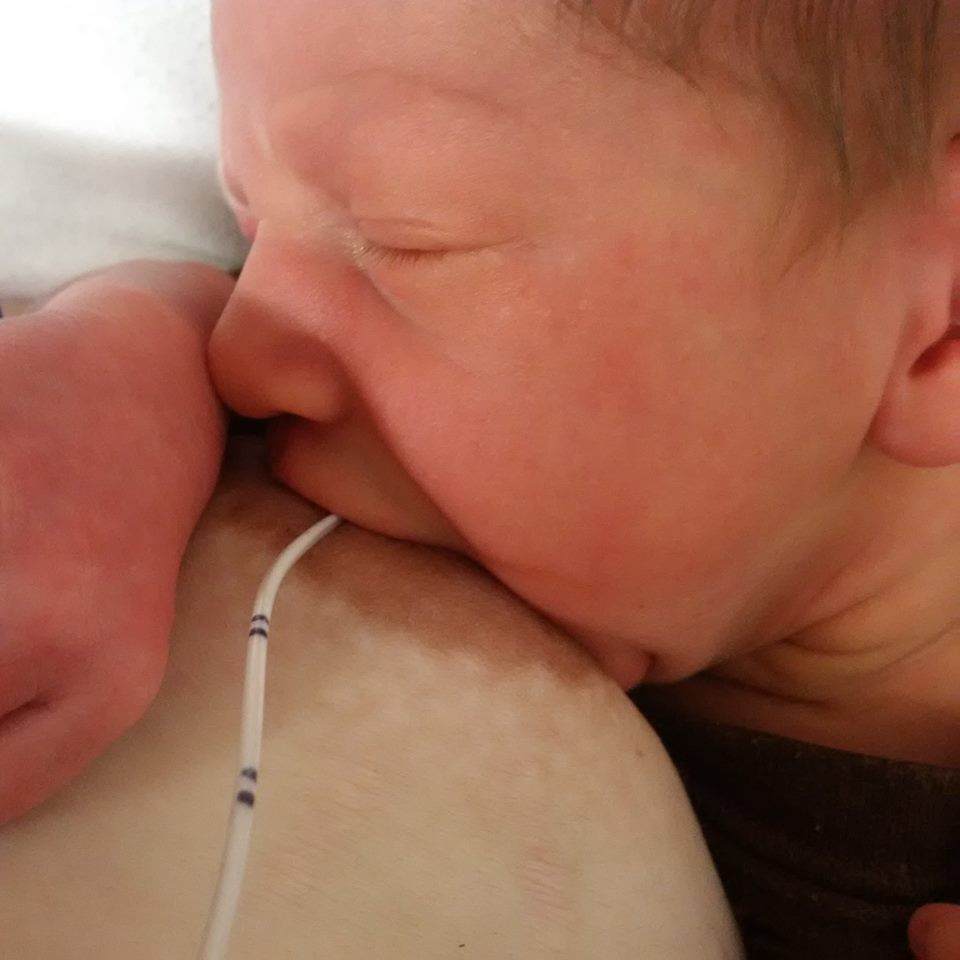
Supplemental Nursing Tube System
There was a point when I thought, “We shouldn’t do this anymore.”
But I didn’t say that because I wanted to support my wife, and she was convinced that breast is best. She believed what she had been told: breastfed babies are healthier, smarter, and better bonded to their mothers than formula-fed babies. I didn’t buy the bonding argument because I knew I was bonding with my baby. I didn’t think our baby would be stunted in any way if she wasn’t breastfed. I think there’s a fine line for a partner between being supportive and being pragmatic, saying that the benefit we are trying to achieve isn’t worth it. I was trying to stay supportive.
At some point during all this struggle, we took the baby for her well-infant exam. The pediatrician was a breastfeeding expert but she gave us formula samples and told us to feed the baby. She told Meredith that the toll breastfeeding was taking on her mental health was not worth the benefit. Meredith was brokenhearted but eventually “gave up” breastfeeding.
I thought it was a weight off everyone and I burned the SNS in the backyard.
We had our second child in 2016. Meredith had never really gotten over “failing” to breastfeed our first, and she was set on breastfeeding our second, too. This baby was different. Our first baby didn’t want to nurse, but our second baby loved nursing, as long as she was awake. But as with our first baby, there just wasn’t enough milk. Our new baby was very sleepy and wanted to sleep more than she wanted to eat.
I could see that Meredith was in excruciating pain every time she nursed. I just held her hand and helped her break the baby’s latch when she needed me to.
We realized breastfeeding wasn’t working when our baby was 3 days old. She wasn’t gaining weight and she had jaundice. The pediatrician gave us formula samples and told Meredith to limit the time the baby was at the breast, so Meredith and the baby wouldn’t get too tired and frustrated. Meredith didn’t listen, though, because she thought she could make it work by “trying harder.” Meredith tried using a nipple shield, which helped the pain but the baby wouldn’t latch on to it. She started pumping again.
Every time she pumped she got angry and upset, because she wanted to hold our baby instead.
We struggled along, with Meredith nursing, pumping, and both of us bottle feeding. One day Meredith’s pharmacist suggested she go to a breastfeeding supply store owned by a lactation consultant. I didn’t want to go because I thought it was a bunch of witchcraft, but I went to support my wife.
The owner sold nursing bras, nursing shirts, nursing pajamas, pumps, cookies, herbs, teas: everything related to breastfeeding that you can think of. The owner suggested we get a weighted feed because the baby got hungry while we were there. She drank less than an ounce of breast milk and was still frantically hungry, so I said I was going to the car to feed her.
When my wife came out to the car a few minutes later, she was in tears .Instead of supporting my wife, the lactation consultant blamed her for her low supply. I told my wife that this woman was wrong, but I couldn’t take away my wife’s shame. My wife paid that woman $100 for lactation cookies, supplements, and a pumping bra that day. I felt it was a waste of money but again, I wanted to support my wife, so I didn’t complain.
My wife was in tears because the lactation consultant told her she was not making enough milk because she was giving formula to the baby and making the baby lazy.
We went to the OB-GYN for my wife’s postnatal follow up and my wife asked why her supply was low and how she could improve it. The doctor suggested trying fenugreek. My wife said that it was her understanding that there was no evidence to support the use of fenugreek to increase milk supply, and the doctor agreed! She said that because my wife was aware of this information, there would be no placebo effect so there was no point in trying it.
The OB-GYN also had her nurse midwife – IBCLC come in to talk to Meredith. She said that it was fine to stop breastfeeding and to use formula, but my wife insisted that she wanted to continue breastfeeding. The nurse midwife-IBCLC advised us that the only ways to increase supply were by pumping (which Meredith was doing) or by taking reglan or domperidone. My wife did not want to take reglan because of the risk of depression. The doctor told us that domperidone is not approved for use in the United States, but we could order it on the internet. I told my wife that she was not going to take sketchy medicine from a sketchy online pharmacy. As much as I wanted to support her, I couldn’t let her risk her health like that. Instead she risked her mental health by taking reglan. While it increased her supply somewhat, it wasn’t enough to justify the risk, and it wasn’t enough to allow her to exclusively breastfeed.
I felt like Meredith was just trying to grab on to anything that would make breastfeeding work, and nothing did. Her friends did not have a supply problem and the lactation consultants acted like there was nothing some herbs or pills couldn’t remedy. Meredith was crushed that she couldn’t provide all the nutrition our baby needed, and she obsessively sought the reasons for low supply.
My wife desperately sought the reasons why she had low supply and there was no evidence based information.
My wife finally found what our family needed when she came across Dr. Christie del Castillo-Hegyi’s letter to doctors and parents about the dangers of insufficient exclusive breastfeeding. Meredith messaged Dr. del Castillo-Hegyi, thanking her, and Dr. del Castillo-Hegyi responded so kindly. She told my wife to hold her head high and be proud that she was giving our baby everything she needed. For the first time in 7 years, someone truly understood my wife’s struggle.
After that, my wife consulted with Jody Segrave-Daly and she helped Meredith build her supply with power pumping so she could get rest and the most enjoyment out of nursing our daughter. Jody also realized that our baby was in danger of falling off the growth chart, and helped us get our daughter’s growth back on track with her expertise of neonatal nutrition.
Dr. del Castillo-Hegyi and Jody Segrave-Daly were the only source of evidence-based breastfeeding support my wife found.
We do not have any pictures of me giving bottles to my children because of my wife’s shame at being unable to exclusively breastfeed. But with the support of the Fed is Best Foundation, Meredith has realized that there’s no more reason to be ashamed of using formula than there is to be ashamed of using contact lenses. My wife felt that her low supply was a reflection on her womanhood and her motherhood, but it isn’t.
There’s a rumor that there’s buried treasure out in the desert somewhere. There’s no evidence of it, only rumors. But people still go searching for it. That’s how it was with recommendations to improve milk supply. The pediatricians and OB-GYNs defer to the lactation consultants, and the lactation consultants all had some story, like “You have low supply because you are using formula.” Or, “You need to use brewer’s yeast and oatmeal.” Or the worst, “Only 5% of women have low supply.( Even 5 % is a significant number for low milks supply! ) Most women have plenty of milk,” as if my wife couldn’t possibly be one of the supposed 5%. All these rumors were being passed off as fact, and there was no evidence for any of them. But my wife believed the rumors because they came from “professionals” who were legitimated by medical doctors.
There’s no telling how much time and effort my wife spent trying to find the mythical buried treasure. I feel sad and frustrated when I think that she could have been spending that time and effort with our family. I feel angry at the doctors who passed my wife off to lactation consultants instead of giving her evidence-based advice. I can’t help but think of the anguish my wife would have been spared had someone before Jody told her, “You probably have low supply. Low supply is real and it isn’t your fault. No amount of trying is going to fix it.”
The thing about being a supportive partner is that you don’t know what it’s like to struggle with breastfeeding. You don’t know how it feels to not be able to provide what everyone is saying you should be able to provide. You don’t know how it feels to not live up to those softly lit, beautiful photos of mothers with flowers in their hair, gazing at their babies while they contentedly nurse. I couldn’t know how my wife felt to “fail” at something that’s supposedly comes naturally to mothers, so I never felt I could give her advice about it or tell her I thought she should let it go. I felt like I could help my wife emotionally, but I couldn’t fix it. The only thing I could do was feed my babies and support her.
I was relieved when my wife found Jody and Christie of the Fed is Best Foundation, because she finally realized that it wasn’t her fault that our first child didn’t want to nurse; it wasn’t her fault that nursing caused excruciating pain; it wasn’t her fault that she had low supply.
No amount of trying harder would have changed our situation, in fact, I think all the trying harder my wife did just made her miserable.
HOW YOU CAN SUPPORT FED IS BEST?
There are many ways you can support the mission of the Fed is Best Foundation. Please consider contributing in the following ways:
- Join the Fed is Best Volunteer group to help us reach Obstetric Health Providers to advocate for counseling of new mothers on the importance of safe infant feeding.
- Make a donation to the Fed is Best Foundation. We are using funds from donations to cover the cost of our website, our social media ads, our printing and mailing costs to reach health providers and hospitals. We do not accept donations from breast- or formula-feeding companies and 100% of your donations go toward these operational costs. All the work of the Foundation is achieved via the pro bono and volunteer work of its supporters.
- Share the stories and the message of the Fed is Best Foundation through word-of-mouth, by posting on your social media page and by sending our resources to expectant moms that you know. Share the Fed is Best campaign letter with everyone you know.
- Write a letter to your health providers and hospitals about the Fed is Best Foundation. Write them about feeding complications your child may have experienced.
- Print out our letter to obstetric providers and mail them to your local obstetricians, midwives, family practitioners who provide obstetric care and hospitals.
- Write your local elected officials about what is happening to newborn babies in hospitals and ask for legal protection of newborn babies from underfeeding and of mother’s rights to honest informed consent on the risks of insufficient feeding of breastfed babies.
- Send us your stories. Share with us your successes, your struggles and every thing in between. Every story saves another child from experiencing the same and teaches another mom how to safely feed her baby. Every voice contributes to change.
- Send us messages of support. We work every single day to make infant feeding safe and supportive of every mother and child. Your messages of support keep us all going.
- Shop and Fed is Best Foundation will earn cash back! We hope to develop our online safe infant feeding classes with these funds.
- If you need support, we have a private support group– Join
We believe all babies deserve to be protected from hunger and thirst every single day of their life and we believe that education on Safe Infant Feeding should be free. If you would like to make a donation to support the Fed is Best Foundation’s mission to teach every parent Safe Infant Feeding, please consider making a one-time or recurring donation to our organization.




Wtf! These poor poor babies ! Feed your damn babies and tell all the lactivists no matter what stupid letters after their names to go shove their titty milk and tubes you know where . No baby deserves to have to go trough this . And these people pushing dangerous drugs and herbals. They’re like drug dealers !
Notice how throughout the narrative, Meredith’s husband remains supportive. He doesn’t tell her what to do or belittle her choices. He validates her feelings. That is the very definition of an ideal partner. So often we hear of women whose husbands contribute to their problems. We need more stories like this one to remind us that for a vast number of women, their partners are their greatest allies.
You are a beautiful person for supporting your wife through all these exhausting trials! My partner and I had our own struggles with breastfeeding our son, and I read this story, I suppose, to feel not alone. We were told so many things before a speech therapist found out that our son has a high arched palette, a mouth shape that made it difficult for him to receive the sensory information of the breast in his mouth and to latch properly. The right profesional makes all the difference. The SNS, along with much pumping, and crying from the baby and myself, eventually worked. Of course that is not the same for everybody! Of course low milk supply is real. It’s as if those lactation consultants who cheated your wife out of her money were suggesting some placebo herb to heal a broken leg in place of a cast, or to say a diabetic should just make enough insulin. When I read about your wife finally being understood, I cried. It makes me hurt to think of the suffering she went through, and I admire her determination so very much. What a strong spirit. I have no doubt your children are both perfectly smart and brave and strong people like their parents.
I am reading this post with my 4 weeks and 2 days newborn girl in my hands. I cannot describe how much I and my wife can relate to this post. We are exactly in the same situation: low milk supply, fenugreek, breastfedding tea, pumping, breastfeeding, formula, and the list goes on. We even tried acupuncture as well! This post helped my wife realize that indeed there is nothing wrong with low milk supply and formula feeding. I will also burn the SNR. I am so fed up with all this. It destroys our happy moments. Not anymore! Cheers from Switzerland.