This is hard for me to write. My breastfeeding experience is a trauma that I don’t like to relive but is undoubtedly the biggest cause of my postnatal depression and anxiety (PNDA). But perhaps I can save someone else unnecessary pain and heartache. I know some will disagree, but hopefully, my story can be a tiny cog in the wheel of feeding guideline reform.
Going into pregnancy, I knew Fed is Best. I decided I would attempt breastfeeding but if it didn’t work out, there’s always formula. Simple. Now, I’m a scientifically minded person. I respect those in the field and the scientific consensus. As I progressed through my antenatal appointments, it became clear. The general consensus is, the breast is best, at all costs, with an inference that ‘formula is dangerous’. By the time my daughter was born, I had made up my mind. If other people formula fed, I wouldn’t judge, but I was going to breastfeed no matter what. I’d get all the help I needed.

My baby began crying from distress after breastfeeding.
That help wasn’t enough. My daughter would breastfeed for up to 3 hours at a time as the pain in her tummy would only allow a tiny bit of milk before she would either start screaming and thrashing in discomfort or fall asleep (probably from low blood sugar). A quick feed would be around 90 minutes. Her reflux also dictated that I had to hold her upright for 30 minutes after a feed, otherwise she’d wake instantly again. I was with her all night every night, with her chewing at my nipple shield on and off, fighting with her to just take a little bit more so I could have more than 2 hours of broken sleep a night. I was beyond sleep deprived. She was only getting enough milk to survive because she was constantly feeding. She barely slept, and was either feeding or screaming, clearly in pain. Once, people came running in a car-park because they thought she must’ve been badly hurt, her screams were that pained.
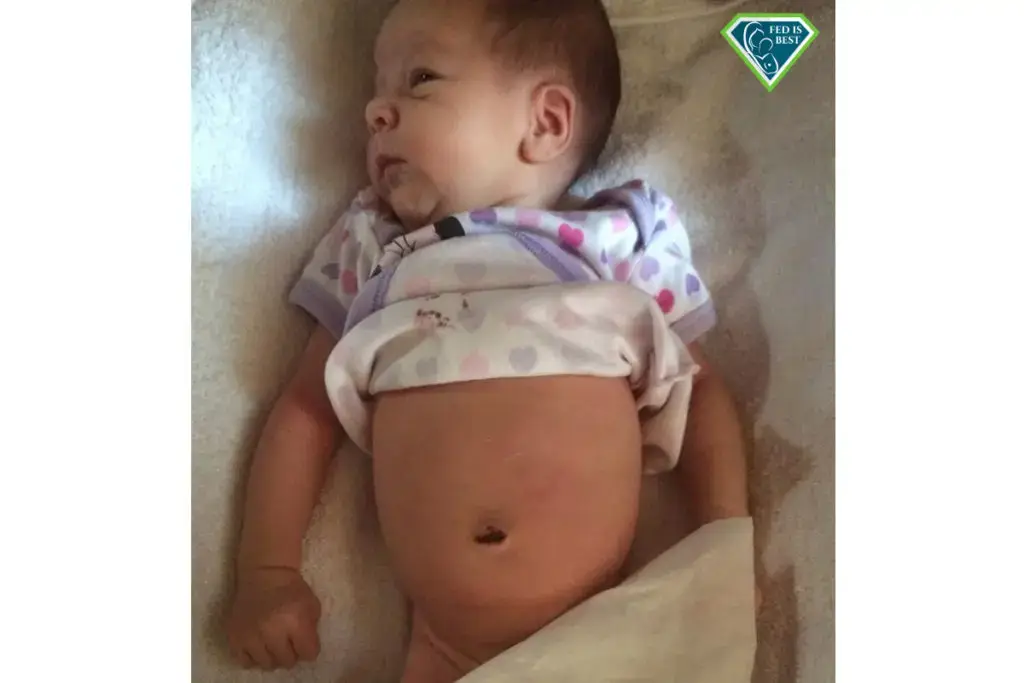
Her stomach was swollen and she was in distress
I’d heard that “the only reason breastfeeding fails is a lack of support” a million times. Lack of breastfeeding ‘support’ was not the problem. The health professionals I saw reiterated that “it’s normal for babies to cry” when I was pleading and crying in their offices. I stayed for 4 nights in the hospital for extra ‘breastfeeding support.’ I went to the breastfeeding drop-in clinic multiple times. I saw an IBCLC and joined a breastfeeding support Facebook group. I called the ABA helpline. I saw my GP. I saw a second GP. I consulted the child health nurses. I rang Tresillian. I sought support on several Facebook pages and subsequently had my daughter’s tongue and lip ties cut, eliminated dairy, soy and minimised salicylates, tried block feeding, bottle feeding expressed breast milk (EBM), gripe water, infants friend, Infacol, infant gaviscon, colic mix, probiotics, baby massage, bicycle legs, patting techniques, babywearing, skin to skin, dummies and eventually prescription reflux medication.
Nothing worked. My nipples were completely ravaged and I started to visually hallucinate from lack of sleep. I feared I was going into psychosis. We even brought up the idea of adoption, because I didn’t know how I could physically go on any longer. I felt I had no attachment to this baby because she was shattering me as a human.
My husband would race home from work to try to get her to sleep for an hour in the baby carrier so I could take a nap, but I had so much anxiety that I’d just lay there and sob uncontrollably. I was severely, severely sleep deprived but my anxiety would not allow me to sleep. The knowledge that I would be up all night, yet again, just broke me every evening. The constant breastfeeding meant that she was completely dependent on my broken, exhausted self. A break was not possible.
I obsessively researched during this time and it became pretty clear that she had an allergy or intolerance of some kind. I read that the most common was dairy, and apparently, that often goes hand-in-hand with soy allergy, so formula wouldn’t solve my problems unless I got my hands on expensive, prescription allergy formula.
I prayed for a way out, or reprieve of any kind.
One evening, when she was about 6 weeks old, I read another mum’s post on one of the Mum’s pages that I’m a member of. She described her baby’s symptoms in detail, which were identical to my daughter’s. Her paediatrician had recommended a specific lactose-free formula to her and it changed her baby overnight. I was at the point of trying absolutely anything, literally for survival purposes, so I messaged my husband to pick some up on his way home.

Six weeks old and struggling to stay at 5 percent on her weight curve.
I was terrified to give it to her. I was scared she had a cow’s milk protein intolerance (even though I eliminated dairy from my diet weeks earlier). I thought it would most likely make her symptoms worse. The words swirled around my mind: “Breast milk is perfectly made for your baby. Formula is too heavy on their delicate stomachs. It will get easier. Formula has no antibodies.” But with the reality that it just couldn’t possibly get much worse, I gave her a bottle.
I woke up to some grizzling, not screaming. I looked at my phone and it was 5.30am. SHE SLEPT THROUGH THE NIGHT!
I shook my husband awake and he didn’t care that I woke him, he was equally as excited. After a quick bottle, she fell back asleep for another few hours. I’ve never felt such relief in my life. She completely stopped screaming, just cried when she was hungry. Otherwise, she was perfectly content and so happy! Over a few days, I completely fell in love with her for the first time. Nobody could believe the change in her. I Iearned that underneath the pain, she had the most joyous spirit. She jumped from the 5th percentile for weight, up to around the 50th and then tracked nicely along that curve as she grew. She was more focused and interested in her environment. We finally bonded.

She is smiling and happy for the first time!
The breastfeeding ‘support’ I received failed me and my daughter. It nearly killed me and my daughter.
Initially, I felt a little guilty about quitting breastfeeding. But sharing my experience led me to a few evidence-based feeding pages. From there I learned that much of the relied upon research touting the benefits of breastfeeding is skewed by confounding factors. Often this is socioeconomic status – there is a correlation between breastfeeding rates and higher socioeconomic status (poorer mother usually needs to go back to work and therefore formula feed). So many of these ‘benefits’ (lower BMI, higher IQ, and many health outcomes) are more likely a result of privilege, not breastfeeding itself. If you’d like to research this further, Google scholar is your friend, or join an evidence-based feeding group if you’re not sure how to critically evaluate research.
But aside from all of that, even if breastfeeding was 100% proven to have better outcomes, a mother is equally as important! The whole family matters! If your other children are suffering because your baby needs you 24/7, that’s a good enough reason to use science milk. If you want your husband or family to join in on the feeding experience, that’s a good enough reason. If you’re struggling with latching or cluster feeding, that’s a good enough reason. If you enjoy bodily autonomy and want your body back, that’s a good enough reason. If you just don’t want to, that’s a good enough reason! There is a correlation between poor breastfeeding experience and postnatal depression and anxiety in new parents. Whatever the reason, mental health is SO important. So whether you breastfeed, mix feed, tube feed, SNS feed, formula feed, or use screened donor milk, you are doing an amazing job. Keeping your baby fed in a loving environment is what truly matters. Besides, they will be licking the floor in 6 months anyway.
I’m still suffering the effects of the pressure to breastfeed nearly 3 years on. I won’t be breastfeeding any future children as the trauma is too great and there is really no need.
People die because of this pressure.
Babies die because of this pressure.
On a final note, I am not bashing breastfeeding. Just the egregious pressure placed upon mothers to breastfeed. I think breastfeeding is amazing if you choose to do it. As long as you do whatever you think is best for your family and personal circumstance, without disregarding your physical and mental health. If you love it and it works for you, go for it! I support you.
To everybody who reads this, please provide a safe space for mother’s to feel no shame in their feeding choice. Support all choices, lives depend on it. ❤
The love in this picture is enormous. We are both thriving for the first time.
If this resonates with you in any way, please share the post.
If you are having a hard time, reach out.
PANDA has a national helpline, 1 300 726 306.
Postpartum Support International
Get Help
PSI Helpline:
1-800-944-4773
#1 En Espanol or #2 English
OR TEXT: 503-894-9453
For safe, evidence-based feeding guidelines visit Infant feeding resources for parents.
Is the “breast is best” mantra an oversimplification?
Clinicians’ Guide to Supporting Parents with Guilt About Breastfeeding Challenges
WAYS YOU CAN SUPPORT FED IS BEST
There are many ways you can support the mission of the Fed is Best Foundation. Please consider contributing in the following ways:
- Join the Fed is Best Volunteer group to help us reach Obstetric Health Providers to advocate for counseling of new mothers on the importance of safe infant feeding.
- Make a donation to the Fed is Best Foundation. We are using funds from donations to cover the cost of our website, our social media ads, our printing and mailing costs to reach health providers and hospitals. We do not accept donations from breast- or formula-feeding companies and 100% of your donations go toward these operational costs. All the work of the Foundation is achieved via the pro bono and volunteer work of its supporters.
- Share the stories and the message of the Fed is Best Foundation through word-of-mouth, by posting on your social media page and by sending our resources to expectant moms that you know. Share the Fed is Best campaign letter with everyone you know.
- Write a letter to your health providers and hospitals about the Fed is Best Foundation. Write them about feeding complications your child may have experienced.
- Print out our letter to obstetric providers and mail them to your local obstetricians, midwives, family practitioners who provide obstetric care and hospitals.
- Write your local elected officials about what is happening to newborn babies in hospitals and ask for legal protection of newborn babies from underfeeding and of mother’s rights to honest informed consent on the risks of insufficient feeding of breastfed babies.
- Send us your stories. Share with us your successes, your struggles and every thing in between. Every story saves another child from experiencing the same and teaches another mom how to safely feed her baby. Every voice contributes to change.
- Send us messages of support. We work every single day to make infant feeding safe and supportive of every mother and child. Your messages of support keep us all going.
- Shop and Fed is Best Foundation will earn cash back! We hope to develop our online safe infant feeding classes with these funds.
- If you need support, we have a private support group– Join


Hello, how long did itbrake for your daughter to reach the 50th percentile? Did you noticed any long term effect after some months or years? I had problems with the breastfeeding for the first 3 months but after she jumped from the 20th to the 80th percentile for both weight and height. She then reached all the milestones even in advance (started walking at 11 months). The only thing I noticed is that her head and face seems smaller compared to other babies and I wonder myself if it is due to the first months problems I had with feeding. Thanks.