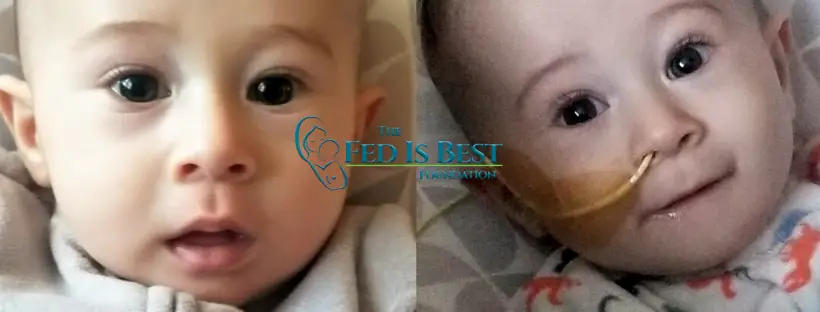
By a Fed is Best Supporter
After having difficulty breastfeeding my older son, I was determined to have a healthier feeding experience the second time around. I learned, through incredible suffering with PPD, that the most important thing was a healthy baby and mother. This time, I had a plan: I was going to give my baby both breastmilk and formula.
My second son was born on his due date. The birth was without complications, and he latched within an hour of being born. I did have some damage to my nipples initially, but we met with a lactation consultant shortly after discharge and she was incredibly helpful. She helped me position my son correctly, and I stopped experiencing pain when he latched. My nipples were healed within a week, and my son regained his birth weight as well. By the time he was two weeks old, he took in 2.5 ounces after about ten minutes of nursing, as measured by a weighted feeding.
To be sure I was successful with breastfeeding, I sought out every resource imaginable. A nurse came to our home for two months, and my son was gaining so well, we were discharged from her services. Every week, she weighed my son, checked his vitals, and tracked his growth. In fact, she was impressed with his weight gain. For a while, he gained over eight ounces a week. He would not take much from a bottle, but nursing was so easy that I really didn’t mind. I was on an extended leave from work and thought we had time to figure out bottle feeding.
Right around this time, my son became extremely gassy with mucousy diapers. He was very fussy and would not sleep well. I had to hold him for all of his naps, his overnight sleep was interrupted, and he was constantly uncomfortable from stomach pain. His head broke out in a scaly rash, and he scratched it so much, he made himself bleed from his fingernails.

Scaly rash from a dairy allergy
I tried block feeding thinking he was getting too much foremilk. I held him upright after every feed and applied various shampoos and creams on his rashes, but nothing helped him. On the day he turned three months old, his pediatrician diagnosed him with a milk protein allergy. I began drastic changes to my diet and tried supplementing with a special formula, but he still was not taking a bottle—even a bottle of breastmilk. He began nursing for shorter periods but more frequently. Eventually, he went from nursing for ten minutes to just four.
At four months old, his pediatrician diagnosed him with failure to thrive. I was devastated. It’s hard to be home with your baby, doing everything possible to feed and love them so they thrive, and then hear the word “failure.” I’m still trying to think of an alternative label. I continued making changes to my diet hoping to provide him relief so he would sleep.
I eliminated all foods known to cause allergies, but it made no difference. I lost 25 pounds. I was not thriving either.

Diagnosed with failure to thrive.
Throughout these challenges, I sought support from the Fed is Best Foundation’s parent support group. The moderators helped ground me when I felt overwhelmed and afraid. The members were wonderful about offering me support for nursing and providing me with tips for bottle feeding. I also began infant feeding consultation with Jody, one of the founders of the Fed is Best Foundation.
After our consultation, Jody suspected that my baby might have a tongue restriction. She sent me back to my pediatrician, who referred me to a pediatric ENT to have a tongue-tie revision. I had relief from the mild pain of nursing, but my baby still did not nurse significantly longer which meant I was still nursing at least every two hours. Jody suggested alternative ways to supplement my son in addition to breastfeeding. I tried an SNS system, a cup, a spoon, and using a syringe. She recommended asking my pediatrician about fortifying my breastmilk with an amino-acid based formula to help him gain weight. My pediatrician agreed and prescribed 24-calorie fortification. His weight gain was minimal, and the conversations with specialists started to include the phrase “feeding tube.” Jody listened to my worries and answered every question I could think of while preparing me for each doctor’s visit.

Diagnosed with a tongue tie by a pediatric ENT physician.
I was afraid. I knew I wanted my son to be healthy, but putting a feeding tube into his body was terrifying. Still, my husband and I were spending so much time trying to get him to eat. We’d try the bottle, then syringe-feed him the formula, and then I would nurse him; we were trying everything to get as many calories into him as possible. He continued to have issues related to his allergy, and I knew my breast milk was still causing him problems. He was weak and stopped rolling over. When he was awake, everything centered on desperate attempts to get him to eat. Then, in early January, he lost weight despite us trying so hard to avoid putting a feeding tube in.
We were seeing multiple doctors and going to appointments all over the state. We were spending all day either feeding him or holding him so he could sleep. We had every resource imaginable. It wasn’t enough.
The next day, his pediatric gastroenterologist admitted him to the hospital. They placed the tube, and we spent five nights there while his team of doctors figured out the right amount of specialized formula to feed him. I pumped for comfort, but I let go of the idea of breastfeeding him. It wasn’t helping him, and I just wanted a healthy baby.

By the time we were discharged, he’d gained over ten ounces. Before the tube, that would have taken three to four weeks.
The day we came home from the hospital, my son started babbling more. His time awake increased. We could play with him, read to him, and spend time together as a family. A month into having the tube, he is rolling over again, sitting up, and is almost caught up developmentally. We began feeding therapy and have seen some small successes in a short time.
I finally see my son thriving. I see him laughing again. Because of the support I received from Fed is Best, we were able to understand that a feeding tube was not a failure. When it came time to get his tube, it was a decision made after careful thought and preparation, rather than one that was made under dire circumstances.
I don’t know what the future holds for my son, but I know he will thrive and grow. I know he will laugh, play, and be the happy baby he deserves to be. That is because he is now thriving while being fed formula, and because we know Fed is always best, including when it’s from a tube.

Finally thriving with love, tube feeding, and complementary foods. #FedIsBest
HOW YOU CAN SUPPORT FED IS BEST
There are many ways you can support the mission of the Fed is Best Foundation. Please consider contributing in the following ways:
- Join us in any of the Fed is Best volunteer and advocacy, groups. Click here to join our health care professionals group. We have: FIBF Advocacy Group, Research Group, Volunteer Group, Editing Group, Social Media Group, Legal Group, Marketing Group, Perinatal Mental Health Advocacy Group, Private Infant Feeding Support Group, Global Advocacy Group, and Fundraising Group. Please send an email to Jody@fedisbest.org if you are interested in joining any of our volunteer groups.
- If you need infant feeding support, we have a private support group– Join us here.
- If you or your baby were harmed from complications of insufficient breastfeeding please send a message to contact@fedisbest.org
- Make a donation to the Fed is Best Foundation. We are using funds from donations to cover the cost of our website, our social media ads, our printing and mailing costs to reach health providers and hospitals. We do not accept donations from breast- or formula-feeding companies and 100% of your donations go toward these operational costs. All the work of the Foundation is achieved via the pro bono and volunteer work of its supporters.
- Sign our petition! Help us reach our policymakers, and drive change at a global level. Help us stand up for the lives of millions of infants who deserve a fighting chance. Sign the Fed is Best Petition at Change.org today, and share it with others.
- Share the stories and the message of the Fed is Best Foundation through word-of-mouth, by posting on your social media page and by sending our FREE infant feeding educational resources to expectant moms that you know. Share the Fed is Best campaign letter with everyone you know.
- Write a letter to your health providers and hospitals about the Fed is Best Foundation. Write to them about feeding complications your child may have experienced.
- Print out our letter to obstetric providers and mail them to your local obstetricians, midwives, family practitioners who provide obstetric care and hospitals.
- Write your local elected officials about what is happening to newborn babies in hospitals and ask for the legal protection of newborn babies from underfeeding and of mother’s rights to honest informed consent on the risks of insufficient feeding of breastfed babies.
- Send us your stories. Share with us your successes, your struggles and everything in between. Every story saves another child from experiencing the same and teaches another mom how to safely feed her baby. Every voice contributes to change.
- Send us messages of support. We work every single day to make infant feeding safe and supportive of every mother and child. Your messages of support keep us all going.
- Shop at Amazon Smile and Amazon donates to Fed Is Best Foundation.
Or simply send us a message to find out how you can help make a difference with new ideas!
For any urgent messages or questions about infant feeding, please do not leave a message on this page as it will not get to us immediately. Instead, please email christie@fedisbest.org.
Thank you and we look forward to hearing from you!