By Julia a. bennett
Today begins the first of a series of posts dedicated to informing parents about infant health conditions related to feeding. We begin with Newborn Jaundice, which comes up frequently in our discussions here at The Fed Is Best Foundation.
Jaundice is not a disease or illness, but the name of a symptom found in babies (and some adults) whose livers can’t clear out a yellow-colored substance called bilirubin (bil-eh-ROO-bin).
Bilirubin is a normal byproduct of red blood cells breaking down in our bodies, which is a normal biological function. Usually, with enough food and liquids and a healthy liver, our livers are able to filter out the bilirubin so we can pass it in our stool and urine. But when our livers can’t clear it out quickly enough, we become “jaundiced,” a word that derives from the french word jaunisse, which means “yellowish.”

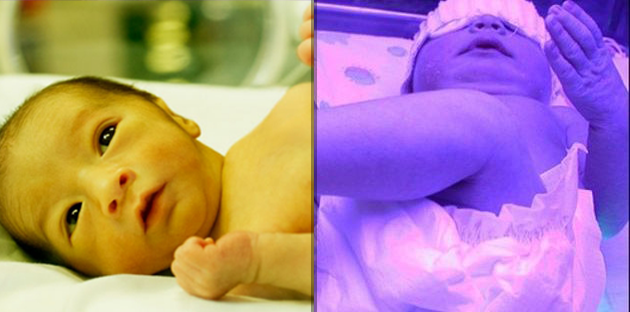
Newborn with yellow-tinged skin from jaundice
As our yellow-colored bilirubin levels rise, our skin and the whites of our eyes take on a yellowish hue.
Jaundice affects 60% of newborns, especially premature babies (earlier than 37 weeks) since their livers aren’t quite ready to keep up with the bilirubin they’re producing. Fortunately, infant jaundice is usually harmless and can be quickly resolved by consuming enough breast milk or formula. Eating and hydrating helps their livers turn the bilirubin into waste and expel it into their diaper.
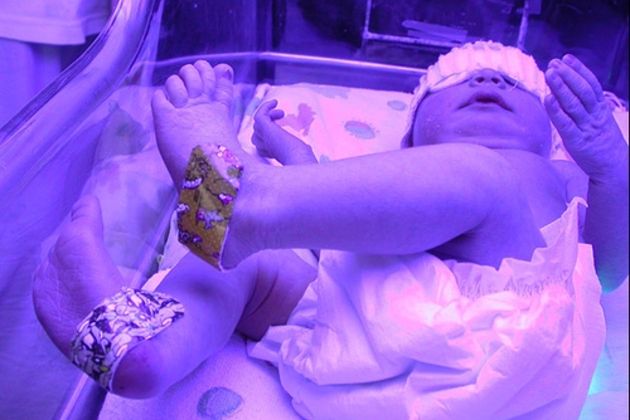
A newborn under a “Bili” Light
When milk intake is not enough, sometimes light therapy (also called phototherapy) is used when the jaundice is more severe. When a baby is carefully exposed to special “Bili” lights in the hospital (which you can see in the adjacent image), it helps break the bilirubin down into a byproduct that the baby can more easily pass.
But we just said that newborn jaundice is harmless, right? Why would the newborn need help getting rid of it if it does no harm? The answer is, bilirubin is harmless only in small amounts. Bilirubin, if excessive, can accumulate in the brain and cause damage. To understand why, you need to know that there are 4 types of newborn jaundice:
- The most common type is physiologic jaundice, which happens for the reasons described above. It’s typically harmless because the levels in the bloodstream are low and so it is easily managed, disappearing after the first week or two of life as an infant’s liver matures and they consume enough breast milk or formula.
- Blood-type incompatibility (hemolytic) jaundice, which happens most often when a mother and baby have different blood types. In the most common scenario the mother’s body produces antibodies that will destroy a newborn’s red blood cells and create much more bilirubin than can be cleared out. This can be very dangerous but can be prevented and treated by your pediatrician / neonatologist.
- Breast-milk jaundice, which happens in a slim percentage of mothers who produce a special substance in their breast milk that typically increases a baby’s bilirubin levels. It can begin around a week of age and last up to 10 weeks with little to no lasting effect on the infant. Bilirubin blood levels are typically stable and not dangerous and continue to decrease as an infant’s liver matures. Your pediatrician will monitor your baby very closely in these scenarios.
- And finally, breastfeeding jaundice, which happens when a baby does not get enough breast milk from their mother to be able to process the bilirubin into their stools and urine. This can happen when they are not latching well or, more commonly, when a mother is not producing enough breast milk in the first days of life. We would like to emphasize that insufficient breast milk production is not the mother’s fault and happens to at least 22% percent of all mothers and 44% of first-time mothers. We refer to this jaundice type frequently here at The Fed Is Best Foundation, and it is estimated that it happens in 10-18% of newborns. It is like physiologic jaundice, however, instead of improving, it worsens as a baby continues to receive insufficient amounts of breast milk. At that point, not only is the baby suffering from starvation and dehydration, but their bilirubin levels are increasing with nowhere to go. This jaundice may appear the same outwardly in that the baby is yellow, but it is dangerous because the bilirubin can start accumulating in places that it can injure. Excessive bilirubin – or hyperbilirubinemia – can accumulate in a baby’s brain and lead to irreversible brain damage.
This last bullet is why it is so imperative to make sure that you supplement your baby’s intake if he or she may not be receiving enough breast milk.
See your baby’s doctor urgently if:
- Your baby seems to not be getting enough breast milk and is constantly crying;
- If you are producing little to no breast milk or colostrum;
- Your baby is very fussy and crying despite breastfeeding for hours.
Get emergency medical help if your baby:
- Is crying inconsolably or with a high pitch;
- Is hard to wake up or will not sleep at all;
- Is very yellow or orange (skin color changes start from the head and spread to the toes);
- Does not have enough wet or dirty diapers**
- Is not breastfeeding or sucking from a bottle well;
- Is arched like a bow (the head or neck and heels are bent backward and the body forward);
- Has a stiff, limp, or floppy body;
- Has strange eye movements
**Additionally, we strongly recommend that all parents who are exclusively breastfeeding their child also weigh them regularly to determine total intake. See our weighing guide and protocol here. For more information about Newborn Jaundice, you can also download this fact sheet from the CDC.
What I do not see posted here are the rates of mothers that are given pitocin that end up with a Jandice baby. I know your site says it is evidence based, but should you also let parents know that the use of pitocin in labor increases the risk of jaundice to begin with?
Maybe breastfeeding and being fed the best would go better if less mothers had unnecessary interventions and drugged up births.
I would like to see the rates of drug free/out of hospital births and jaundice vs hospital births/inductions etc to see if there is a correlation.
Exclusive breastfeeding and insufficient milk intake are actually the most significant predictors for developing excessive jaundice because bilirubin is removed through milk passing through the gut. There is no scientific evidence that pitocin increases jaundice levels in newborns.