Para leer en español, por favor vaya aquí.
When our son was born, he weighed 6 pounds 5 oz., and we had issues with him latching from the start. Part of the problem was I had flat nipples, so the nurse gave us a shield and showed me how to use it, and he seemed to do much better. He seemed to be a very content and alert baby. He lost almost 10 percent of his birth weight during our hospital stay, and we were discharged to see our pediatrician for a follow-up.
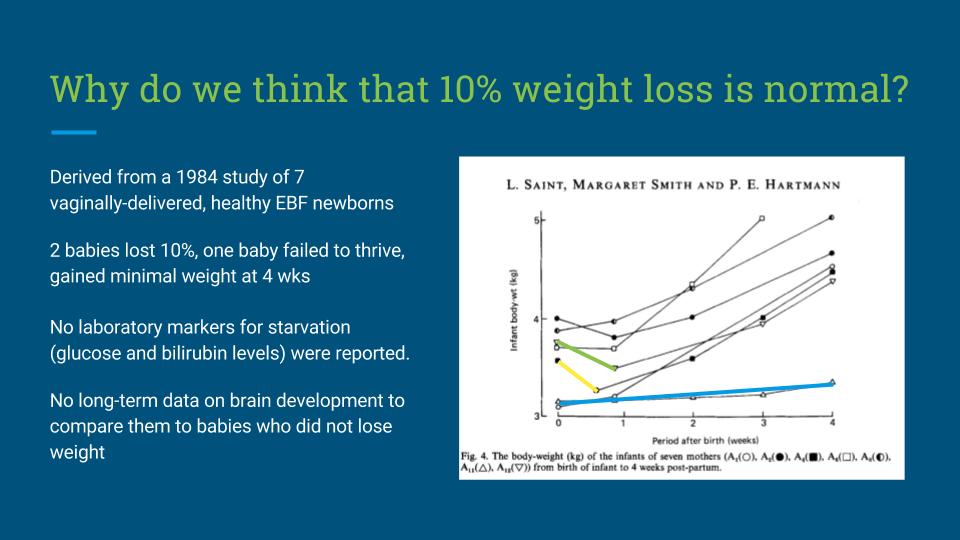
We continued to use the shield because he struggled to latch without it and were told to put it back on if he got frustrated trying to latch. I noticed that the shield would be full of milk when he finished. I also noticed that he wanted to eat for very long periods of time and didn’t seem ever to be settled during or after feeds.

My friends in Facebook mommy groups said this was pretty typical behavior and that he was just cluster feeding, so I continued to let him eat as often as he wanted, for as long as he wanted. I also never felt like my milk came in, at least not how my friends had described it. He didn’t get back up to his original weight by his 1-week visit, but the doctor didn’t seem overly concerned at that point because he had wet and dirty diapers.
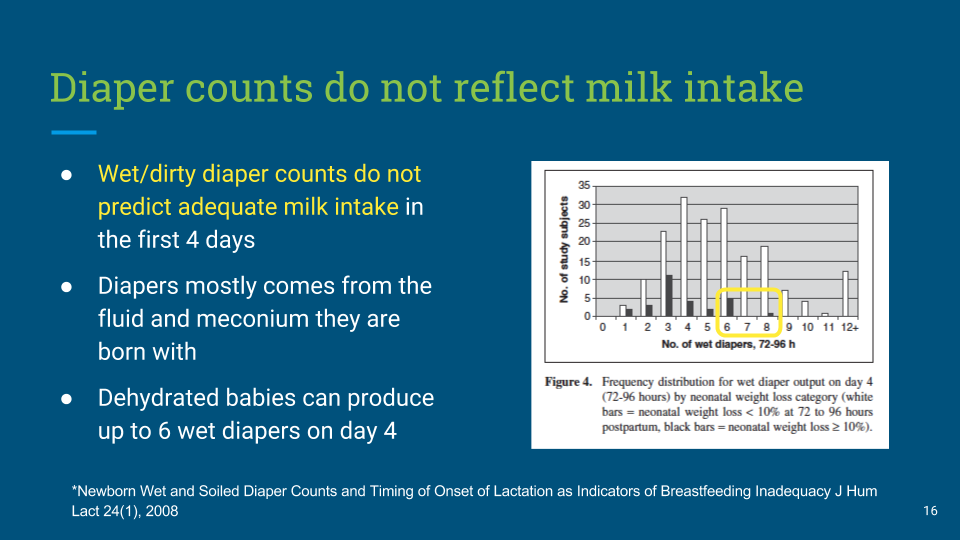
At his 1 month appointment he only weighed 6 pounds 5.5 ounces. He had only gained ½ of an ounce and his pediatrician suggested I talk to the lactation consultant.
I went the next day to a group class, but the class was so large that I felt very overwhelmed and left early. I decided to attend the class offered at the hospital where he was born, where two of the nurses we met would be teaching the class. They had me first weigh him, feed him, and then weigh him again. When we weighed him after his hour-long feeding, the lactation consultant told me he had only eaten 20ml!

She suggested I start supplementing with formula and put me on a pumping schedule to try and increase my supply. We went home and immediately began the routine, and at the next week’s visit, he had gained nearly 2 pounds.
The nurse’s response was, “Wow! He must have been hungry.” He wasn’t just hungry, he was starving!
We continued the routine, and he continued to grow and thrive, but my supply didn’t seem to be increasing, and he still seemed so restless while nursing. The restlessness turned into full-on screaming after he nursed or drank a bottle of breast milk. I called his doctor, and she said it sounded like he had reflux. She prescribed Zantac and suggested that I cut dairy out of my diet. I met with my doctor for my 6-week postpartum checkup and told her about having to cut out dairy. She had experienced the same thing, so she sat down with me and went over things I could and couldn’t eat and what to look for on food labels. I also had a friend who did the same thing, so I followed her food plan, but he still would get so upset when he had any breast milk. After nearly a month of pumping every two hours, not eating, not sleeping, and trying to grieve the loss of my father, who had passed away two weeks before our son was born, I was an emotional mess.
My mom called me one day, and I was on the verge of a mental breakdown when she said, “he needs you to be healthy and sane far more than he needs breast milk.” At that moment, I felt a little bit of weight lift off my shoulders. I made an appointment to talk to his doctor about not breastfeeding. I had difficulty accepting it and worried that she might push me to keep breastfeeding.
Her beautiful response:
“You’ve tried harder than 99% of the moms I’ve worked with to make breast feeding work, and it’s totally OK if you stop and exclusively formula feed.”
I cried in my doctor’s office because that was the validation and permission I was looking for. I tried so hard to breastfeed my baby, but it was certainly not what was best for either of us. By his two-month appointment, he had more than doubled his weight, and at six months, he is back to being a happy, observant, content baby and so far meeting his milestones right on schedule.

Formula saved my baby’s life!
I have felt so guilty, and it took a tremendous amount of courage for me to write my story. At the same time, I am so thankful my baby is now thriving and feel it is extremely important for other moms to understand that if your baby is not gaining weight, it is critical to figure out why and not assume everything is normal, no matter what popular breastfeeding mom groups on Facebook might say!
Bottom line: I could have lost my baby and my own sanity. For me and my baby, #fedisbest
I will be forever grateful for finding the Fed Is Best Foundation, and I am now committed to working with their advocacy team to promote #SafeBreastfeeding.

My story one year later. What I learned.
I had countless moms—some that I knew personally, many I did not—send me messages thanking me for having the courage to share and for saying the things they were too ashamed to admit. I had a mother message me and tell me, “these were the words I so desperately needed to hear right now.” I had friends and family message me to say that their friend or family member from another state had shared our blog and how proud they were to tell them that they knew me. I had friends message me that they never truly believed that there were mothers who “couldn’t breastfeed” until they read my story.
I Shared My Story a Year Ago And I Was Told To Go Kill Myself – How I Am Healing
For more information on protecting your baby from feeding complications due to early exclusive breastfeeding, please read and download the Fed is Best Feeding Plan, a way to communicate your feeding choices to your health care providers.
In addition, please read and download the Fed is Best Weighing Protocol to prevent newborn dehydration and failure to thrive.
To learn how to supplement your baby:
How To Prepare For Supplementing When Breastfeeding Your Baby In The Hospital
Feeding Your Baby—When Supplementing Saves Breastfeeding and Saves Lives
.
Lastly, please watch our educational videos on Preventing Feeding Complications for more detailed information.
Our full list of parent resources can be found on our Resource Page.
HOW YOU CAN SUPPORT FED IS BEST
There are many ways you can support the mission of the Fed is Best Foundation. Please consider contributing in the following ways:
- Join the Fed is Best Volunteer group to help us reach Obstetric Health Providers to advocate for counseling of new mothers on the importance of safe infant feeding.
- Make a donation to the Fed is Best Foundation. We are using funds from donations to cover the cost of our website, our social media ads, and our printing and mailing costs to reach health providers and hospitals. We do not accept donations from breast- or formula-feeding companies, and 100% of your donations go toward these operational costs. All of the Foundation’s work is achieved via its supporters’ pro bono and volunteer work.
- Share the stories and the message of the Fed is Best Foundation through word-of-mouth, by posting on your social media page, and by sending our resources to expectant moms that you know. Share the Fed is Best campaign letter with everyone you know.
- Write a letter to your health providers and hospitals about the Fed is Best Foundation. Write them about feeding complications your child may have experienced.
- Print out our letter to obstetric providers and mail them to your local obstetricians, midwives, and family practitioners who provide obstetric care and hospitals.
- Write your local elected officials about what is happening to newborn babies in hospitals and ask for legal protection of newborn babies from underfeeding and the mother’s rights to honest, informed consent on the risks of insufficient feeding of breastfed babies.
- Send us your stories. Share with us your successes, your struggles, and everything in between. Every story saves another child from experiencing the same and teaches another mom how to feed her baby safely. Every voice contributes to change.
- Send us messages of support. We work daily to make infant feeding safe and supportive of every mother and child. Your messages of support keep us all going.
- Shop and Fed is Best Foundation will earn cash back! We hope to develop our online safe infant feeding classes with these funds.
- If you need support, we have a private support group– Join
We believe all babies deserve to be protected from hunger and thirst every single day of their life, and we believe that education on Safe Infant Feeding should be free. If you would like to donate to support the Fed is Best Foundation’s mission to teach every parent Safe Infant Feeding, please consider making a one-time or recurring donation to our organization.


So brave of you to share this.
I unapologetically formula feed. Formula has liberated me and my breasts. I like sharing the burden of feedings with my partner. I like knowing how much my baby is getting and that I don’t have to count diapers. I also like sleep and the occasional glass of wine… Breast might be best for some mothers but to me ‘Formula is Supreme’. Ironically, the way I feed my baby makes me a horrible mom in the eyes of many. However, to me, choosing formula has allowed me to be the happy and engaged mother that my baby deserves. I was simply too distraught and tired when attempting breastfeeding. I would compare the
difficulty level of breastfeeding to rubbing sticks together in order to make fire. It can be done but, for the love of god, just hand me a lighter.