Written by: Allison Stillwell Young, RN, BSN, Graduate Student and Team leader of the fed is best foundation mental health advocacy team
is an oncology nurse at Vanderbilt-Ingram Cancer Center in Nashville, Tennessee. A graduate of Belmont University, she has spent her entire nursing career between research oncology and behavioral health. After the birth of her older son, she developed anxiety and depression directly related to difficulties she experienced with breastfeeding including low supply and feeding judgment. She discovered Fed Is Best during her recovery from PPD/A and found the Foundation to be indispensable when feeding her younger son. As a researcher and mother living with chronic mental illness, she believes that the treatment for perinatal mood disorders should have evidence basis, and she therefore co founded a large, online pro-science peer support group for those experiencing PMADs in 2016. She sits on the board for the Tennessee chapter of Postpartum Support International and functions as one of their state support coordinators for the Midstate.
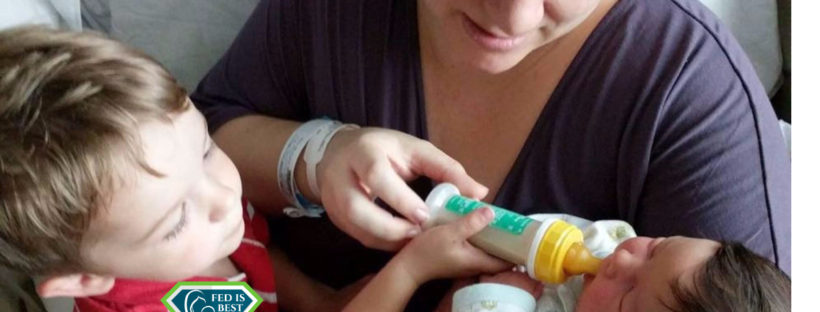
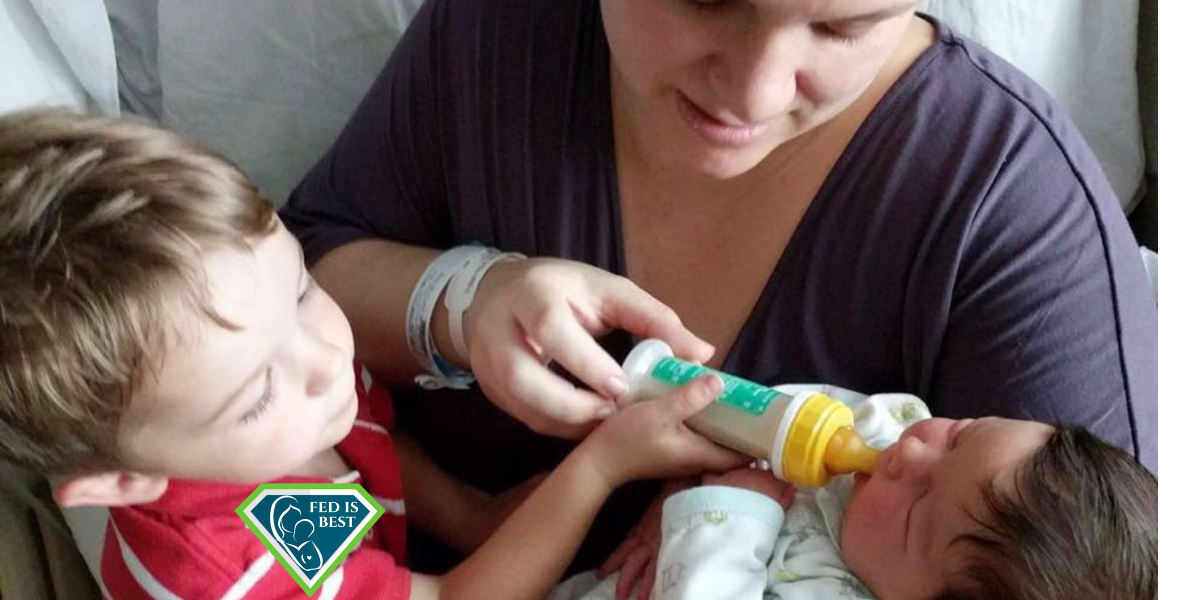
I had our second child last Monday. Since that evening, we’ve been supplementing with formula due to the fact that I have insufficient glandular tissue (IGT) and I am not physically able to exclusively breastfeed. Yesterday, our older son wanted to help feed his baby brother a bottle and, while he was helping, my husband took this picture of them that I loved. I made it my profile picture, and the fact that I felt comfortable posting a picture of my sons with a bottle really shows a sea change in my feelings about infant feeding. Because of that picture, I wanted to post my story about lactivism, which is extremist exclusive breastfeeding advocacy, and how it affected my postpartum mental health after my older son’s birth. It’s pretty long, but I hope my story illuminates how The Fed is Best Foundations provides important support for new mothers.
Prior to my Soren’s birth, I really drank the “breast is best” Kool-Aid. I was absolutely convinced that it was the only acceptable way to feed a baby, and that moms who didn’t breastfeed were lazy. At no point did anyone in my birthing or breastfeeding classes tell me that lactation failure was even a thing, and it wasn’t something I learned in nursing school either. I mean, looking back, as someone who has an autoimmune disorder and two long-term mental illnesses, I should have recognized that the breasts are able to fail just like any other part of the body, but it just didn’t cross my mind at all.
A couple of weeks before Soren was born, I went to a lactation consultant to be fitted for a nursing bra, and the lactation consultant asked if I’d had any changes in my breasts during the pregnancy. I had. So I said “yes” and she left it at that.
Later, she would tell me that she recognized I had markers for IGT but that she didn’t want to scare me, so she withheld this important clinical information from me.
After Soren’s birth, it seemed like he was doing an okay job feeding, but he kept dropping weight. He was jaundiced, but not enough that treatment would be indicated. Even though his weight kept dropping and dropping, I was never offered any formula or safe, screened, and pasteurized breast milk to increase his weight. I only heard placations that weight loss was normal in a breastfed infant. His pediatrician almost didn’t discharge him on my last day at the hospital, but I begged her to let me take him home because I didn’t want to be separated from my baby.
On March 11, 2015, he was born at 9 lbs, 2 oz. By his five day appointment on March 16, 2015, he weighed 7 lbs, 14 oz. When his pediatrician did a weighted feed in the office, he didn’t consume enough over a 40 minute feeding for any milk in his belly to even register on the scale. My husband gave him a formula nursette in the office and he guzzled it so fiercely that he immediately vomited it back up. He was starving.
I was absolutely devastated. Despite my family 100% supporting me and reminding me that my husband and I were both exclusively formula fed, and my son’s pediatrician and my obstetrician holding strongly “fed is best” beliefs, the Facebook mom groups were strong in their vehemence against formula and they tainted my mind. I was convinced I was poisoning our child. These judgmental lay people told me over and over again that my care team, which included two International Board Certified Lactation Consultants (IBCLC), lied to me and that lactation failure is so incredibly rare that there was absolutely no chance that I had it. These women blamed me for my IGT even after my IBCLC/WHNP (Women’s Health Nurse Practitioner) told me that IGT was genetic and could not have been avoided.
I had people tell me directly that I should not be allowed to have children if I am not able to breastfeed exclusively or that my infant son should be taken from me for the same reason. I’ve seen other women told that if their children starve, it is natural selection and that babies should be allowed to die if their mothers can’t breastfeed them.
It wore me down. I became obsessed with trying just one more supplement, one more food, one more dose of domperidone—despite knowing the effects this medication could have on my heart. I had worked in drug development, and I knew that domperidone could affect my heart’s electrical cycle. At one point, I was taking ten different pills that promised increased milk production, not even bothering to check if any of them interacted with my other medications or were safe for my infant son. I was a woman possessed. I obtained huge amounts of unscreened donor milk, eschewed formula, and tracked my pump output at work better than I had ever tracked anything in my life.
By nine months postpartum, my anxiety was at absurd levels. Despite the fact that our son was thriving, it still hurt me deeply every time I fed him a bottle. When I was driving to work one day, I realized I had conceived a suicide plan and that horrified me. My inability to exclusively breastfeed had been a constant destructive force in my life since my son’s birth. My psychiatrist was able to help me greatly by changing my medications and providing the therapy I needed to pull me out of the darkness, but it still hurt.
It wasn’t until Jody Segrave-Daly, a co-founder of The Foundation, came into my life that I really truly began to heal from the cruelty I’d been subject to from other mothers. The creation of the Fed Is Best Foundation and their commitment to evidence-based practice and research highly appealed to me as a healthcare professional and combination feeding mom. They helped me recognize that feeding my child safely was all that mattered, and they gave me the strength to be as open with my feeding struggles as I’ve been about my struggles with mental illness.
The day that I scheduled the birth of my second son, Rune, I called the lactation department at my hospital and made it clear that we would be combination feeding and that I needed a lactation consultant to come immediately after birth to institute formula supplementation. The lactation consultant who answered the phone was incredibly supportive and sweet. Then, when Rune was born, the lactation consultant on call was the same one who had withheld knowledge about my IGT markers when my older son was born. She refused to bring a supplemental nursing system (SNS) for me as I’d requested. Thankfully, the baby nurse and my postpartum nurse were glorious. They both supported my supplementation, and immediately stocked me well with formula.
Yesterday, my husband took a picture of our sons that I loved. When I had Soren two and a half years ago, I absolutely refused any picture of me feeding him unless I was breastfeeding. There are no pictures of me feeding him formula because I was embarrassed. It made me feel like a bad mom. Yesterday, however, when Soren asked to feed his brother, I didn’t even hesitate as my husband took pictures of this sweet moment with my two precious boys. When I saw the picture my husband posted, I immediately made it my profile picture because it made my heart feel so full.
There is nothing wrong with feeding my child. There is nothing wrong with formula. Women who feel superior are ableist, misogynist, and victim-blaming all at the same time. They are disrespectful and, frankly, they don’t care about moms or babies.
Don’t let these people get to you. Breastfeeding is not the be-all and end-all of motherhood. Your baby needs you more than breast milk (a fact that is lost in the world of lactivism). Nurturing doesn’t come from breast milk—it comes from you. Bonding doesn’t come from a breast—it comes from you.
Please take care of yourselves. Don’t fall down the hole like I did. Healing is possible—this picture shows that—but it’s better if you never feel that pain at all. We support you however you feed your baby and we feel that your mental health is absolutely paramount. You are not distilled down to a body part. You are a person with needs, and your choices should be respected.
Much love to all of you who have also been hurt by lactivism. Please know that you’re absolutely safe here.
The Fed Is Best Foundation has a private Facebook support group and we welcome all families: Support Group Screening
Allison’s Facebook Support Group: Perinatal Mood and Anxiety Disorders Pro-Science Peer Support Group
HOW YOU CAN SUPPORT FED IS BEST
There are many ways you can support the mission of the Fed is Best Foundation. Please consider contributing in the following ways:
- Join the Fed is Best Volunteer group to help us reach Obstetric Health Providers to advocate for counseling of new mothers on the importance of safe infant feeding.
- Make a donation to the Fed is Best Foundation. We are using funds from donations to cover the cost of our website, our social media ads, our printing and mailing costs to reach health providers and hospitals. We do not accept donations from breast- or formula-feeding companies and 100% of your donations go toward these operational costs. All the work of the Foundation is achieved via the pro bono and volunteer work of its supporters.
- Share the stories and the message of the Fed is Best Foundation through word-of-mouth, by posting on your social media page and by sending our resources to expectant moms that you know. Share the Fed is Best campaign letter with everyone you know.
- Write a letter to your health providers and hospitals about the Fed is Best Foundation. Write them about feeding complications your child may have experienced.
- Print out our letter to obstetric providers and mail them to your local obstetricians, midwives, family practitioners who provide obstetric care and hospitals.
- Write your local elected officials about what is happening to newborn babies in hospitals and ask for legal protection of newborn babies from underfeeding and of mother’s rights to honest informed consent on the risks of insufficient feeding of breastfed babies.
- Send us your stories. Share with us your successes, your struggles and every thing in between. Every story saves another child from experiencing the same and teaches another mom how to safely feed her baby. Every voice contributes to change.
- Send us messages of support. We work every single day to make infant feeding safe and supportive of every mother and child. Your messages of support keep us all going.
Thank you so much from the Founders of the Fed is Best Foundation!
Maternal Mental Health Feels Like it Comes Second to Breastfeeding When It Should Be First
https://fedisbest.org/2017/09/i-made-an-informed-decision-to-formula-feed-my-baby-and-it-was-perfect-for-us/


Thank you for sharing your story! I have IGT and was so grateful that my midwife diagnosed me at 8 weeks pregnant so I had my entire pregnant to come to terms and plan. I requested a lactation constant the day my son was born and she hooked me up with formula and SNS. She was great. Otherwise I’m sure I would have had a very similar story as yours. I never realized until much later that many women do not get this diagnosis until something is amiss with the baby’s weight. I would love to see regular breast screenings for this in pre natal care. It’s was a game changer for me.