by Christine K.
When the Fed Is Best Foundation launched two years ago, a few nurses sent us messages about their experiences working in a Baby-Friendly Hospital Initiative (BFHI) hospital. They shared common concerns about watching exclusively breastfed babies crying out in hunger from not enough colostrum while being refused supplementation just so that high exclusive breastfeeding rates were met. Two years later, we now receive messages from nurses, physicians, lactation consultants, and other health professionals, regularly. They express their concerns while asking for patient educational resources. They tell us their stories and they need support and direction on what to do about unethical and dangerous practices they are forced to take part in. We collected their stories and are beginning a blog series on health professionals who are now speaking out about the Baby-Friendly Health Initiative (BFHI) and the WHO Ten Steps of Breastfeeding.
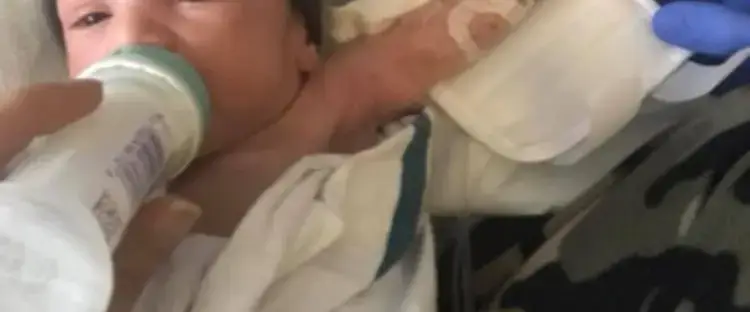
Christine K. is a Neonatal Nurse Practitioner currently working in a BFHI Hospital with 25 years of experience. She has worked in both BFHI and non-BFHI hospitals and talks about her concerns about taking care of newborns in the Baby-Friendly setting.
Regarding Unsafe Skin-To-Skin Practices
In BFHI facilities, skin-to-skin is mandated. The protocol calls for skin-to-skin at birth, for the first hour, then ongoing until discharge. New mothers are constantly told that it is important for bonding, for breastfeeding, for milk production and for temperature regulation of the newborn. Baby baths are delayed for skin-to-skin time and nurses are required to document in detail the skin-to-skin start and end times. There is no education on safety regarding skin-to-skin time, only that it is to be done. I have been responsible for the resuscitation of babies who coded while doing skin-to-skin. One died, and the other baby is severely disabled. Mothers are not informed of the risks of constant and unsupervised skin-to-skin time. Mothers have complained to me that they felt forced to do skin-to-skin to warm up their cold or hypoglycemic infant because they are told skin-to-skin time will help their infant resolve these issues when in fact it doesn’t. There is also no assessment of the mother’s comfort level with constant skin-to-skin. It’s very discouraging to hear staff say things like, “That mother refused to do skin-to-skin,” like it was a crime or an act of child abuse. The judgment is harsh on mothers who fail to follow the protocol. I have noticed that partners are pushed to the side, especially in the first hour of life, not being able to hold their newborn, due to this strict policy. Their involvement has been discounted in the name of the exclusive breastfeeding protocol. Continue reading →